Steppage Gait: Causes, Treatment & Rehab Options
Walking should feel automatic. When it does not, even simple daily activities can become exhausting and unsafe. One common but often misunderstood walking abnormality is steppage gait. This is a compensatory walking pattern frequently linked to foot drop and neurological conditions.
For patients, caregivers, and clinicians, understanding the steppage gait pattern, its causes, and evidence based rehabilitation strategies is essential for restoring safe, efficient mobility.
What Is Steppage Gait?
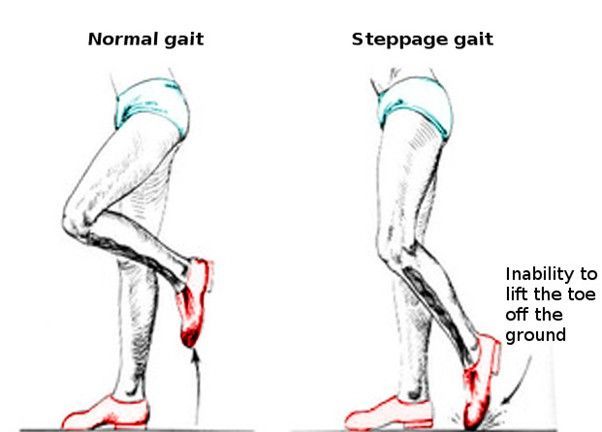
Steppage gait is a walking pattern characterized by excessive hip and knee lifting during the swing phase in order to prevent the toes from dragging.
It is often referred to as high steppage gait and typically occurs due to weakness or paralysis of the ankle dorsiflexor muscles.
Key Features of the Steppage Gait Pattern
- High knee lift during the swing phase
- Toes dragging without compensation
- Foot slapping on ground contact
- Often unilateral with one side affected
Steppage Gait vs Foot Slap
Although related, steppage gait and foot slap represent two different compensations.
| Feature | Steppage Gait | Foot Slap |
|---|---|---|
| Cause | Dorsiflexor weakness | Mild dorsiflexor weakness |
| Swing Phase | Excessive hip and knee lift | Normal swing phase |
| Initial Contact | Often forceful contact | Audible slapping sound |
| Severity | Moderate to severe | Mild to moderate |
Foot slap may be an early sign of progression toward foot drop related steppage gait.
Steppage Gait Causes
The most common causes of steppage gait involve nerve or neurological damage affecting ankle dorsiflexion.
| Cause Category | Conditions Associated with Steppage Gait |
|---|---|
| Neurological Causes | Stroke, Multiple sclerosis, Parkinson's disease, Traumatic brain injury, Peripheral nerve injury such as peroneal nerve damage |
| Musculoskeletal Causes | Lumbar radiculopathy, Post surgical nerve irritation |
Steppage Gait Muscles Affected
The primary muscles involved include:
- Tibialis anterior
- Extensor hallucis longus
- Extensor digitorum longus
Weakness in these muscles prevents normal foot lift and results in compensatory hip and knee flexion.
In cases of steppage gait after stroke, disruption of central motor control delays or reduces dorsiflexor activation during the swing phase.
Steppage Gait in Parkinson’s Disease
Steppage gait in Parkinson’s disease is less common but may occur due to several factors:
- Bradykinesia
- Reduced motor timing
- Impaired proprioception
Unlike the typical Parkinsonian
shuffling gait, steppage gait in Parkinson’s usually reflects focal dorsiflexor weakness rather than generalized slowing of movement.
Steppage Gait Physical Therapy Options
Effective physical therapy for steppage gait focuses on several rehabilitation strategies.
Strengthening
- Targeted dorsiflexor exercises
- Resistance band ankle lifts
- Seated toe raises
Gait Retraining
- Repetitive swing phase training
- Step over drills
- Functional walking tasks
Neuromotor Re education
- Task specific repetition
- Sensory feedback integration
- Proprioceptive training
Orthotic Support
An ankle foot orthosis, commonly called an AFO, may assist in severe foot drop related steppage gait cases. However, braces provide passive support and do not retrain neuromotor walking patterns.
Neuromotor Rehabilitation with Just Walk
For patients seeking active rehabilitation beyond bracing, the Walking Rehabilitation Device Just Walk offers a mechanical wearable neuromotor training solution distributed by Chaban Medical in partnership with Salute Rehab Ltd.
How It Supports Steppage Gait Rehabilitation
- Assists foot lift at step initiation
- Provides adjustable resistive forces with four levels
- Reinforces neuroplastic motor patterns
- Enables structured training sessions lasting approximately fifteen to twenty minutes
Unlike passive braces, Just Walk integrates into the full gait cycle while supporting strengthening and neuromotor reconsolidation during functional movement.
Learn more here:
https://www.chaban-medical.com/just-walk-page/
Comparison: AFO vs Neuromotor Training Device
| Feature | AFO Brace | Just Walk |
|---|---|---|
| Passive Support | Yes | No |
| Active Muscle Engagement | Minimal | Yes |
| Neuroplastic Training | No | Yes |
| Adjustable Resistance | No | Yes |
| Home Integration | Limited | Designed for daily functional activities |
For patients recovering from steppage gait stroke or peripheral nerve injury, combining clinical therapy with home-based neuromotor repetition may enhance outcomes.
When to Seek Evaluation
Consult a healthcare provider if any of the following occur:
- Toe dragging happens regularly
- Falls increase
- Weakness develops suddenly
- Symptoms appear after stroke or nerve injury
Early intervention improves long term walking recovery.
Summary
Steppage gait is more than a cosmetic walking abnormality. It reflects underlying neuromuscular dysfunction. Whether caused by stroke, nerve damage, or neurological disease, early and targeted rehabilitation is essential.
Structured strengthening, gait retraining, and neuromotor repetition, including wearable mechanical training devices, may help patients regain safer and more efficient walking patterns.
Related Topics
FAQ
?What causes steppage gait
Steppage gait causes typically include nerve damage, stroke, multiple sclerosis, and peripheral neuropathy that affect ankle dorsiflexion.
?Is steppage gait the same as foot drop
Foot drop often leads to steppage gait, but mild dorsiflexor weakness may initially appear as foot slap before progressing.
?Can steppage gait improve
Yes. With appropriate strengthening, neuromotor retraining, and physical therapy, many patients experience significant improvement.
?Do braces cure steppage gait
Braces provide support but do not retrain neuromotor control. Active rehabilitation is required for long term improvement.
Sources & References
- National Institute of Neurological Disorders and Stroke (NINDS)
- American Physical Therapy Association Clinical Practice Guidelines
Important
This article is for informational purposes only and is not a substitute for professional medical advice; always consult your doctor or physical therapist before starting any exercise or using any device